The definition of scours is diarrhea, but diarrhea alone only means the calf has loose feces. The important question when a calf has diarrhea is whether it is making the calf sick.
“It’s not as simple as saying, the calf has diarrhea, therefore, it has scours. You need to compare groups of observations, consider the age of the calf and think about the disease pattern on the ranch before making treatment decisions,” says Dr. Frank Garry, department of clinical sciences, Colorado State University.
Read Also

Body condition, nutrition and vaccination for brood cows
One of the remarkable events of the past century related to ranching has been the genetic evolution of brood cows….
A common thread throughout his talk at the University of Calgary’s beef cattle conference was that if you are just randomly treating for anything, you will be misusing medications, can’t expect the same outcomes, and likely won’t adjust calving management to prevent problems in the future.
Garry’s first rule of thumb is, if you can’t catch a baby calf that has diarrhea, it probably isn’t sick and the problem will resolve on its own without treatment. Diarrhea can be a sign of a simple digestive upset from taking on too much milk at one time or eating things that can’t be digested, but check the calf again later to see if its condition has changed.
One of the early signs of sickness is a lack of activity and strength, in which case simple scours should top the list of suspects because the agents that cause it are so common in the environment and notoriously infectious. One or a combination of rotavirus, coronavirus and the protozoa, cryptosporidium is the usual culprit.
Healthy cows and heifers periodically shed these infectious agents in their manure, more so during times of stress such as inclement weather. The pathogens don’t survive long in dry, sunny environments, but when picked up by a calf immediately start multiplying in the gut. Some infected calves never look sick. Perhaps they have a certain level of immunity or natural resistance that gives them the upper hand. Even so, they are walking incubators shedding bugs everywhere they wander, at a rate up to 50 million oocysts and one billion viral particles per gram of feces. On it goes to another calf and another until the environment becomes so contaminated it is nearly impossible for young susceptible calves to escape being sick.
Calves sick at seven to 14 days of age are probably infected with cryptosporidium and/or rotavirus. You might see coronavirus in calves up to a month old, and it tends to be the most aggressive because it damages the large and small intestine.
“All of these calves have basically the same problem. These bugs injure cells on the microvilla lining of the gut causing localized, superficial damage, meaning that they don’t spread beyond there,” Garry explains. “They pour out fluids through the intestine, losing electrolytes and because they lose electrolytes, the blood and body fluids become acidic. The infections don’t kill them. It’s the loss of fluid and electrolytes and acidosis that kills them. Without treatment they won’t last much longer than a day.”
Fortunately, dehydration can be easily treated with proper electrolyte fluid therapy. The gut will repair itself and the prognosis is actually very good for these calves.
The degree of dehydration will determine whether treatment with oral electrolyte fluids is enough or the calf needs intravenous therapy.
Telltale signs of dehydration are tight skin and sunken eyeballs caused when fluid is lost from supporting fat tissues. A pinch to the skin on the eyelid or the neck normally slides back into place in a second or two, whereas tight skin will stay tented for five seconds and longer as dehydration worsens. A gap between the eyeball and bottom eyelid will be noticeable and widen as dehydration becomes severe.
Fluid loss also reduces blood volume and blood pressure resulting in pale eyeballs and gums, and cold ears, tail, and feet.
These calves won’t have fevers unless other complications, such as pneumonia, set in.
Pulling all the signs together, a calf that has lost six to eight per cent of its body fluids is mildly to moderately dehydrated. It is able to stand, may swagger a bit as it walks, be visibly depressed with drooping ears and lowered head, have tight skin, sunken eyeballs, a dry mouth and nose, and the suckling reflex could already be weakening.
Garry says two litres of oral electrolyte solution is a good starting point for treating a baby calf at this stage. Twelve hours later, if the calf is still looking off and easy to catch, give it another two litres. Don’t worry if you can’t catch a calf for followup treatments because this is a good sign that it is on the mend. If the calf looks frumpy again the next day, give it another two litres. Continue feeding two litres of electrolyte solution twice a day about 12 hours apart until the calf is doing well. That could be one day or it might take three days before the diarrhea runs its course.
Garry strongly recommends feeding oral electrolytes by bottle for two reasons. If a calf is so weak it has no suckling reflex, you are way behind already and the calf needs intravenous therapy, or, something else is wrong, in which case dumping fluid into the rumen with an esophageal feeder would really make matters worse. If a sick calf still has a reasonable suckling reflex, use your discretion as to whether bottle or tube feeding would be best.
There’s a fine line between moderate and severe dehydration as the loss of body fluids reaches 10 per cent. The calf won’t be able to stand and all of the other symptoms will be very apparent. If not treated intravenously, the calf will soon slip into a coma. Major organs will start to shut down as cells throughout the body continue to dry out and die.
Treatment with antibiotics won’t help calves with simple scours and is likely to slow the recovery because antibiotics kill good bacteria that aid digestion as the gut heals. Oral antibiotics given when the gut isn’t functioning as it should will be detrimental.
A calf’s gut can be disturbed, but it will get by as long as you keep replacing the fluids and electrolytes lost in the diarrhea, Garry stresses.
Electrolytes are minerals capable of separating into positive and negative ions to carry electrical impulses. The body normally keeps the ions in balance inside and outside of cells so body fluids, blood pressure, nerves and muscles function as they should.
A good-quality electrolyte product for calves will include the two important electrolytes, chloride and potassium, along with sodium to help retain fluids. The alkalinizing agent to correct the acidosis can be either bicarbonate or acetate. Both effectively improve blood pH; however, acetate is preferred because it is a normal product of ruminant digestion and won’t disturb abomasal pH.
Electrolyte products don’t contain all the nutrients a calf needs. Even high-energy electrolytes with glucose have only about half the amount of energy as whole milk. If a calf isn’t suckling the dam, provide two litres of milk per feeding spaced in between the electrolyte feedings. Always mix electrolyte powder with clean water as directed on the label, not with milk.
Inflammatory enteritis
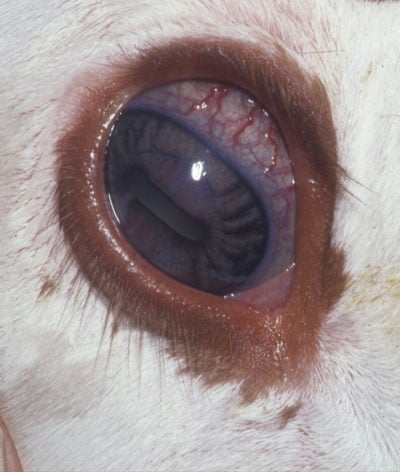 The outcome isn’t very rosy for baby calves with diarrhea due to inflammatory enteritis. This disease is caused by bacteria, the big three being salmonella, invasive types of E. coli, and clostridium.
The outcome isn’t very rosy for baby calves with diarrhea due to inflammatory enteritis. This disease is caused by bacteria, the big three being salmonella, invasive types of E. coli, and clostridium.
They strike calves as young as a few days old up to a month and are vicious because they attach to the gut and excrete endotoxins.
“This is a whole different deal. They beat the dickens out of tissues, invade past the gut and kill calves in completely different ways. Once they break down the tissue barrier and get into the bloodstream they can go anywhere in the body — kidneys, liver, brain, lungs, muscles, joints,” Garry explains.
These systemic infections can be worse than the gut infection itself and the body’s defences against the endotoxins create inflammation that can be as damaging as the bug itself.
Approximately 30 per cent of calves that are systemically ill have a condition known as septicemia because poison from endotoxins has spread throughout the body affecting multiple organs and causing widespread inflammation.
The transfer of passive immunity has failed in most septicemic calves.
The telling sign of bacterial inflammatory enteritis is a high fever rather than diarrhea.
While some calves will show diarrhea, many get so sick so quickly they never develop diarrhea. Garry says the first effects on the gut are so profound the gut stops functioning altogether, causing a condition known as ileus. The abdomen descends as fluids build up in the gut because nothing is moving through. It’s not unusual to hear fluids sloshing around in the gut and a necropsy soon tells the tale as fluid pours out.
A buildup of air (bloat) in the abomasum is a sure sign of clostridium.
Calves with inflammatory enteritis may become somewhat dehydrated and acidotic if they have diarrhea or fluids gathering in the gut. The mucous membranes will be red and inflamed and blood vessels in the white of the eyeball will be bright red and bulging slightly as blood starts to pool due to the effects of bacterial toxins on blood flow.
“You now have a distinction between dehydration signs and inflammatory disease signs. Electrolyte fluid therapy might help rehydrate and correct the acidosis in calves with bacterial enteritis, but because the gut isn’t working, it really is only useful if given intravenously to support cardiovascular function,” Garry explains.
A case could be made for the use of an appropriate antibiotic, he says, but only if given by injection or intravenously. Again, oral antibiotics will do nothing more than set the calf back because they disturb the gut flora and function. An antibiotic will attack the bacteria to stop the release of endotoxins, but won’t counter the endotoxins themselves, nor the damage they’ve already done. Often, by the time you see this disease, antibiotic therapy will be ineffective from the get-go. It may save some, but not many.
Injectable non-steroidal anti-inflammatory drugs such as Banamine and meloxicam may be helpful insofar as reducing fever, pain and swelling caused by the inflammation, but they won’t treat the cause of the disease.
There are no good trials with conclusive evidence to say that home remedies from the medicine cabinet and kitchen pantry are helpful. These are generally over-the-counter prepared and natural products people might take for digestion-related problems. In short, it’s important to discuss these types of supportive therapies with your veterinarian because they can have negative side effects, especially in light of the fact that they are given orally when gut function is already disrupted.
In summary, Garry says, “If a calf has simple scours with the main problems being diarrhea and dehydration and you treat it early when fluid loss is mild to moderate with good fluid therapy, you should see a very good response. If the response is poor and the calf is severely depressed and fevered with signs other than diarrhea, it’s best to call your veterinarian because you are in for a bad storm, probably not with a great outcome. You need to break the rampant infectious cycle or you won’t win with these calves.”
Preventing the storm

Having good records on the numbers of calves that have been treated, with what, their ages, symptoms and outcomes may be all the information your veterinarian needs to pinpoint the most likely pathogen(s) involved, recommend effective treatments and offer a strategy to prevent a full-blown outbreak.
Veterinarians might collect blood and/or fecal samples from sick calves to confirm the initial diagnosis. When calves are dying, necropsies are the most valuable diagnostic step. If it’s not feasible to have a veterinarian necropsy calves all the time, ask him or her to teach you the basics. It’s a simple, straightforward procedure on a baby calf that only takes 15 minutes, Garry adds.
Prevention is a balancing act between minimizing exposure and maximizing resistance.
Maximizing resistance starts long before calving with proper vaccinations and nutrition for the cows to ensure healthy calves and adequate colostrum for effective transfer of passive immunity.
Scours vaccines for immunizing cows and heifers during the last trimester do a good job of boosting antibodies in the colostrum against some viruses and bacteria. Their effectiveness really comes down to the dam’s ability to produce quality colostrum and the calf’s ability to consume enough of it within the first few hours of life.
“What prevents simple scours and enteritis is proper hygiene,” Garry stresses. The proof is in several very good studies showing that scours rarely occurs during the first two to three weeks of a calving season because it takes time for the pathogen load in the environment to build to the point where potentially deadly infections become inevitable.
The Sandhills calving system, so named because it was formally described by researchers at Nebraska-Lincoln University, combines two important elements of prevention: calving in areas without manure buildup and separating pairs according to the age of the calves. Cows stay put in the pasture or corral where they calve and every week those that haven’t calved are moved to clean ground. The number and sizes of the pastures or corrals and frequency of the moves can be adapted to your herd size and resources, always keeping in mind the general idea of grouping calves of roughly the same age to prevent older infective calves from passing the pathogens to younger susceptible calves. Pairs can be regrouped after the youngest calf in the groups to be commingled is four weeks old. The long-standing recommendation to calve heifers apart from cows still holds because heifers’ calves are most at risk of getting sick.
More details on the Sandhills calving system can be found online.

















